Blurred Vision? It Could Be More Than Just Tired Eyes — How Diabetes Affects Your Sight

“I started noticing occasional blurring… I thought I just needed more rest.”
Many people know that diabetes affects blood sugar levels, but fewer realise it can also impact vision. In the early stages, changes may seem mild, slighty blurring, occasional floaters, or difficulty focusing at certain times of the day. Because these symptoms can come and go, they are often dismissed as fatigue or eye strain. However, over time, uncontrolled diabetes can affect different parts of the eye and lead to more serious complications if left untreated. Let’s understand how diabetes affects eye health together with Dr Nazila Ahmad Azli, Consultant Ophthalmologist and Oculoplastic Surgeon at Sunway Medical Centre Velocity, and why early care is essential in protecting your vision.
How Diabetes Affects the Eyes
Diabetes can affect the eyes in several ways, mainly by damaging small blood vessels and altering the normal structure of eye tissues. Persistently high blood sugar levels can weaken these vessels, cause fluid leakage, and reduce oxygen supply to important parts of the eye. Over time, this may lead to vision problems or permanent damage if not detected early. According to Dr Nazila, individuals with diabetes are at higher risk of developing several eye conditions, especially when blood sugar levels are not well controlled.
Common Eye Conditions Linked to Diabetes
Three main eye conditions are commonly associated with diabetes: cataracts, glaucoma, and diabetic retinopathy.
Diabetes and Cataracts
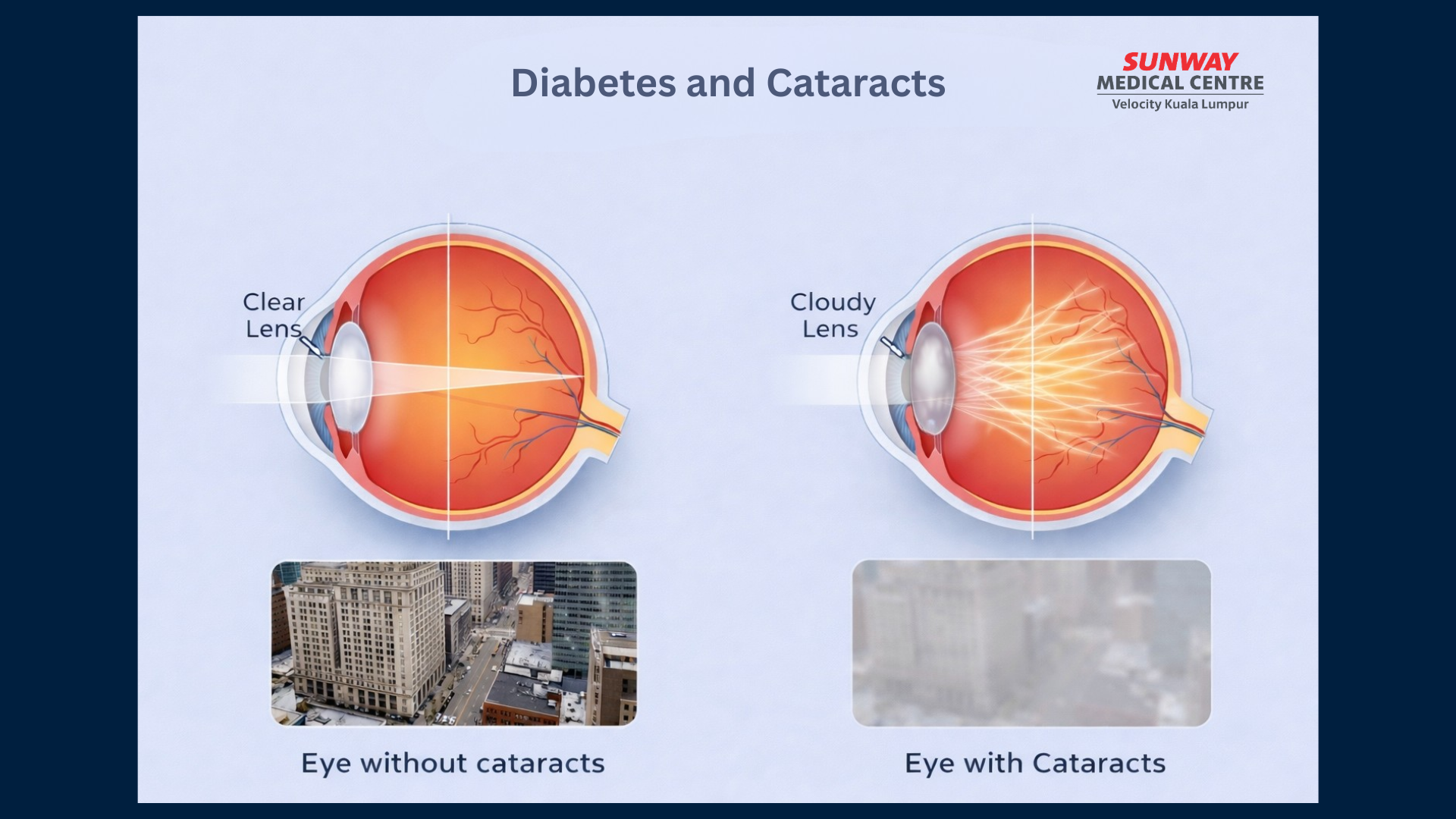
A cataract occurs when the normally clear lens of the eye becomes cloudy, leading to blurred or dim vision. Patients may notice that their vision gradually becomes hazy, or that lights appear more glaring, especially at night. While cataracts are often associated with ageing, people with diabetes may develop them earlier and experience faster progression due to changes in the lens caused by high blood sugar levels. When vision begins to affect daily activities, cataract surgery can help restore clarity by replacing the cloudy lens with an artificial one.
Diabetes and Glaucoma
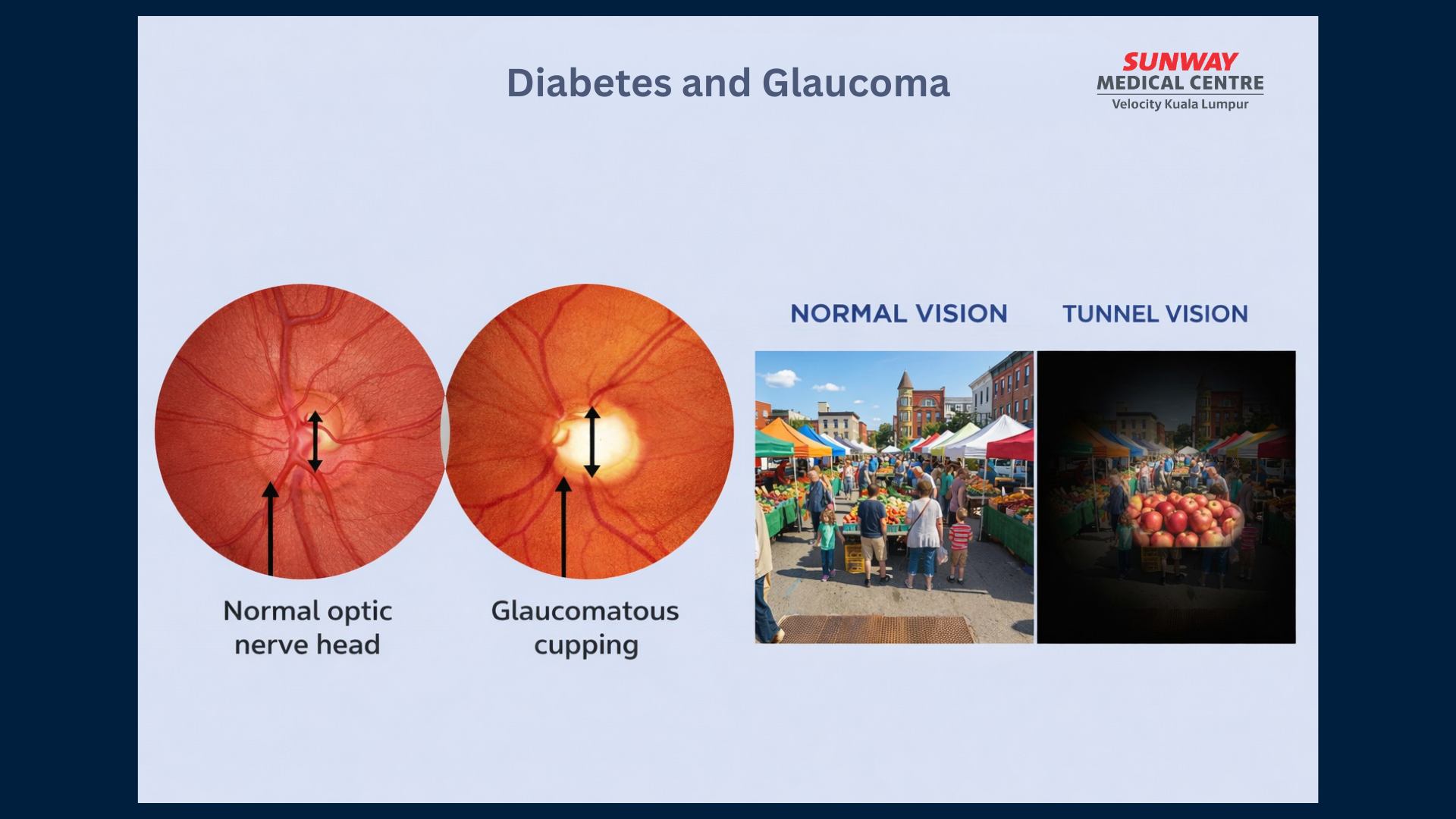
Glaucoma refers to a group of eye conditions that damage the optic nerve, often due to increased pressure within the eye. In its early stages, glaucoma may not cause noticeable symptoms, which is why it can go undetected until vision is affected. People with diabetes are at higher risk, including more complex forms such as neovascular glaucoma, where abnormal blood vessels interfere with normal fluid drainage. Early detection is key. Treatment may involve medications, laser therapy, or surgery, depending on the severity of the condition.
Diabetes and Diabetic Retinopathy
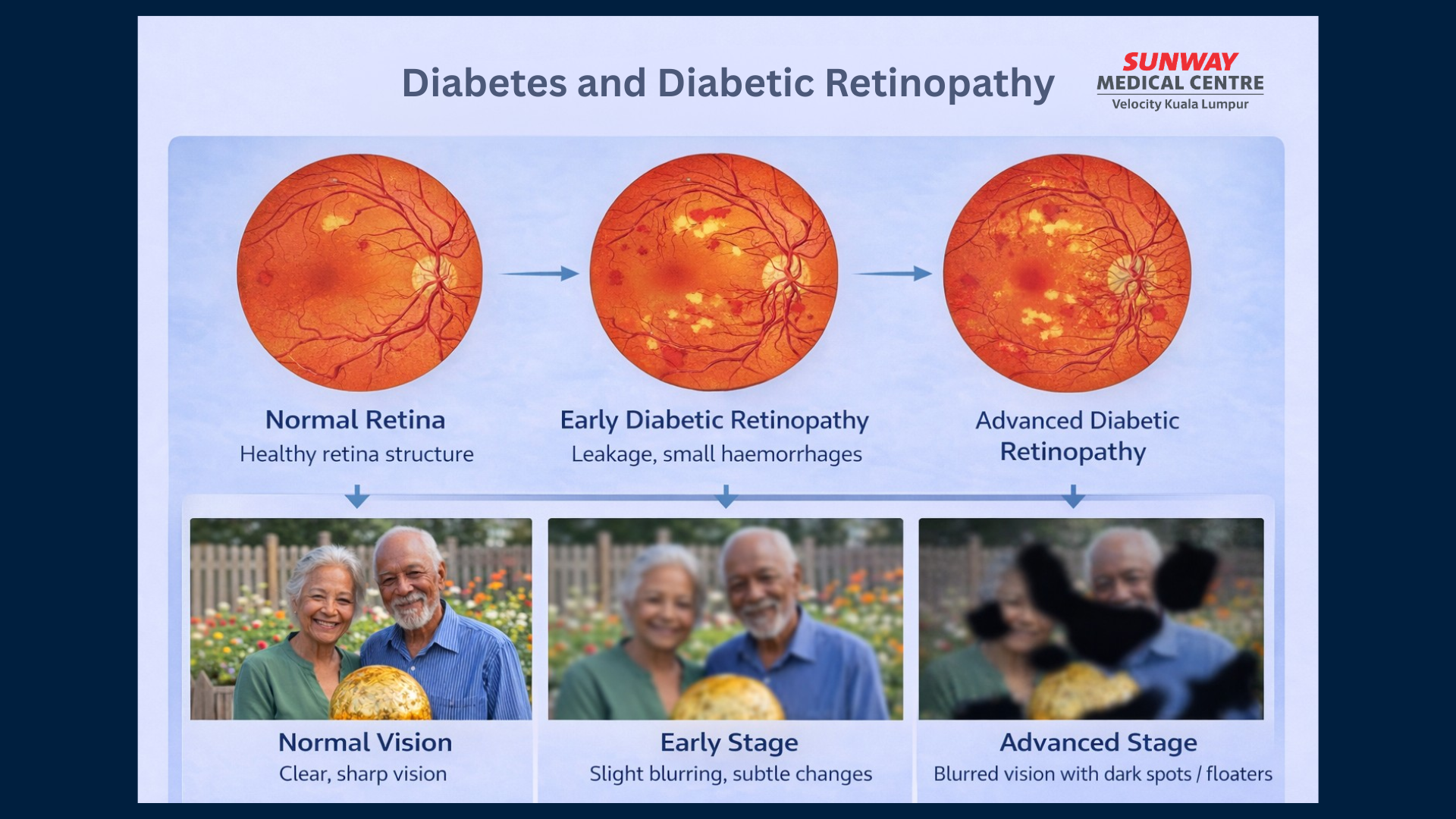
Diabetic retinopathy is one of the most serious complications and a leading cause of vision loss among working-age adults. It develops when high blood sugar damages the small blood vessels in the retina. In the early stages, there may be no symptoms, which is why many patients remain unaware. As the condition progresses, symptoms such as blurred vision, floaters, or dark spots may appear. In more advanced stages, abnormal blood vessels can form and bleed, increasing the risk of significant vision loss.
Regular Eye Screening Is Important
Diabetic eye conditions can develop silently. Many patients only seek help when vision becomes noticeably affected, by then, the condition may already be more advanced. Regular dilated eye examinations allow early detection, even before symptoms appear, significantly improving the chances of preserving vision. Patients with diabetes are advised to have their eyes checked at least once a year, even if their vision feels normal.
Protecting Your Vision: What You Can Do
Managing diabetes effectively plays a key role in protecting your eyes. Keeping blood sugar levels stable helps reduce damage to delicate blood vessels. Monitoring HbA1c, along with controlling blood pressure and cholesterol, is equally important. Healthy lifestyle choices, including balanced nutrition, regular physical activity, and avoiding smoking, can also make a meaningful difference over time.
Treatment Options for Diabetic Eye Conditions
Treatment depends on the type and severity of the condition, with the goal of slowing progression and preserving vision. For diabetic retinopathy, options may include eye injections to reduce swelling and prevent abnormal vessel growth, laser therapy to control leakage, or surgery in more advanced cases. With early detection and proper care, many patients are able to maintain stable vision and continue their daily activities.
Taking a Proactive Approach
Diabetes does not always lead to vision loss. With proper management, regular screening, and timely treatment, many complications can be prevented or controlled effectively. If you have diabetes and notice changes in your vision, even mild or occasional, it is important not to ignore them.
At Sunway Medical Centre Velocity, Dr Nazila Ahmad Azli, Consultant Ophthalmologist and Oculoplastic Surgeon provides comprehensive eye assessments and personalised care to help detect early changes and protect your vision.
Because sometimes, what feels like a small change may be your eyes asking for attention.
Was this article helpful?
1 out of 1 found this helpful
Suggest to Read